A game changer in hormone health.

Salivary diagnostics offer a clearer picture of hormone levels.
Dr. Joe Klassen ND, Medical Director at Rocky Mountain Analytical
Accurately assessing hormone levels is essential to understanding endocrine health, supporting the diagnosis of conditions such as hypothyroidism, hyperthyroidism, adrenal insufficiency and reproductive hormone disorders, as well as for shaping effective treatment strategies. Many hormone measurements can be performed using serum, urine and saliva testing, and each method presents its own strengths and weaknesses. Serum testing remains the most familiar clinical approach for measuring total hormone concentrations, although the results can be influenced by the substantial proportion of hormones bound to carrier proteins that are not biologically active. Urine testing provides valuable insight for assessing hormone metabolites over time, but 24-hour collections can be inconvenient for patients and prone to compliance issues. Saliva testing complements these methods, offering a highly practical option that directly captures the freely available hormones that diffuse into tissues and drive biological effects. With its non-invasive collection, good stability, and decades of validation, salivary analysis has become a dependable and clinically meaningful tool for modern hormone evaluation.
Saliva as a matrix for free hormone measurement.
Hormones circulate in the body in both bound and unbound forms, with the majority of steroid hormones in serum being protein-bound and inactive. The remaining free fraction available to act on tissues is difficult to measure directly and must be estimated indirectly through calculations. In contrast, hormones enter saliva by passive diffusion through the acinar cells, which allow free steroid hormones to pass while blocking conjugated and protein-bound forms. As a result, salivary measurements reflect only the fraction of hormone that is biologically active. Saliva hormone testing also offers practical benefits, as collection is simple, comfortable for patients and easily repeatable, making it ideal for real-time monitoring of hormones that fluctuate throughout the day or month. Unlike blood draws, saliva collection does not introduce stress-related artifacts and does not require clinical supervision, both of which can affect cortisol.
Saliva samples can be conveniently collected at home and shipped without complex preparation, making saliva-based testing well suited to dynamic protocols – such as diurnal cortisol rhythms – or serial measurements across the menstrual cycle. This flexibility enables clinicians to capture hormone patterns in the patient’s everyday environment instead of isolated moments in the clinic, providing a more accurate outline of diurnal hormonal fluctuations. Building on these practical advantages, saliva testing has been validated for more than 50 years, with studies demonstrating strong reproducibility and excellent agreement with patient symptoms. Its most widespread use is in the assessment of adrenal function, where accurate timing and minimal stress during collection are essential.
Diagnosing and monitoring adrenal disorders.
Cortisol exhibits a distinct daily rhythm, with a sharp increase before and after waking, a gradual decline through the day and evening. Saliva sampling enables clinicians to track this pattern at multiple time points without the influence of venipuncture or anticipatory stress, offering a reliable picture of everyday adrenal behavior. This approach is particularly useful in spotting adrenal patterns linked to diseases. Abnormally elevated cortisol during the night may be indicative of Cushing’s syndrome, while consistently low values throughout the day point to an Addison-type presentation. Disrupted rhythms seen in shift workers, persons with PTSD or individuals under chronic stress can affect energy, sleep, metabolic health and insulin sensitivity.
Salivary cortisol for identofying adrenal function.

High and low levels of many hormones, such as prolactin or thyroid hormones, can present with overlapping symptoms including fatigue, mood changes and infertility. This ‘Goldilocks phenomenon’ means that symptom-based assessment alone is unreliable. Serial salivary measurements help clinicians to determine whether hormone levels are too high, too low, or poorly timed, guiding more informed and tailored treatment decisions.
Tailoring informed hormone care.
Saliva testing is particularly valuable for therapeutic monitoring in bioidentical hormone replacement therapy (HRT), where topical or mucosal delivery can bypass first-pass liver metabolism. Serum tests may underestimate tissue exposure because they assess total circulating hormone, whereas saliva measurements reflect the biologically active fraction, with validated reference ranges that reflect observed levels in healthy and affected populations available.
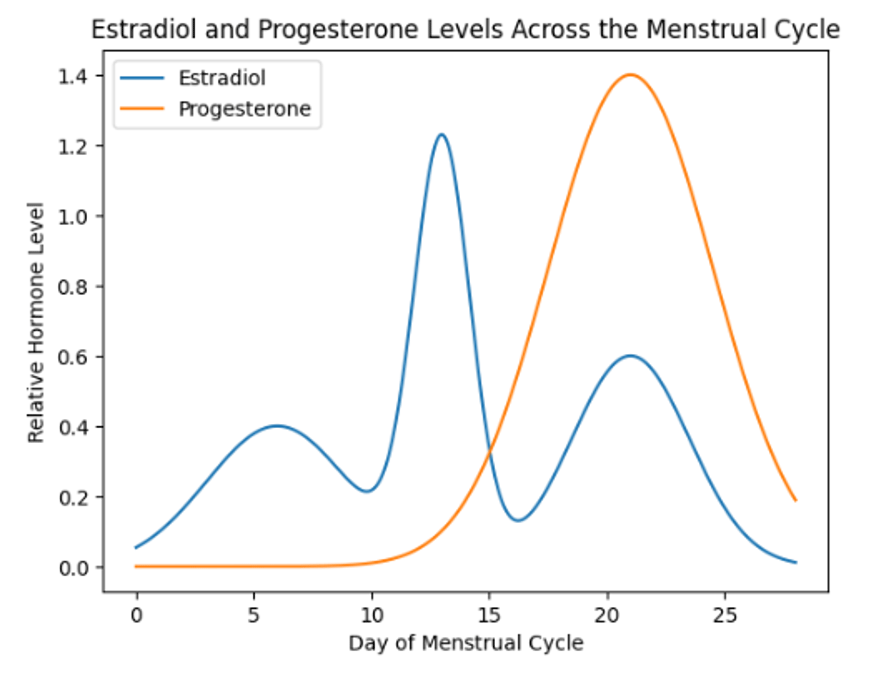
Progesterone monitoring is especially informative for both women and men, given its role in balancing estrogen and supporting reproductive health. In women, serial salivary testing across a full monthly cycle reveals a characteristic hormonal pattern: a rising and falling ‘M-shaped’ curve for estradiol, and a pronounced increase in progesterone following a healthy ovulation. Tracking these cycles can highlight luteal insufficiency or follicular abnormalities that may affect conception. In a clinical example, a 32-year-old woman who struggled to conceive despite regular cycles was found to have significantly low luteal-phase progesterone following salivary testing, despite serum tests suggesting normal hormone levels. Supplementing oral micronized progesterone from day five of her cycle onward resulted in a successful pregnancy within two cycles, and similar success with a second pregnancy two years later. Saliva testing is equally useful for assessing hormones in men, particularly when serum concentrations of estradiol or progesterone are near the lower detection range of traditional assays. Monitoring progesterone in aging men can provide insight into prostate health, as this hormone has protective effects against estrogen-associated enlargement of the prostate.
| Hormone | Status | Result | Range |
|---|---|---|---|
| Estradiol | Within range | 3.5 | 1.0-9.0 |
| Progesterone | Below range | 28 | 50-250 |
| Testosterone | Above range | 51 | 15-45 |
| DHEA-S | Above range | 9.4 | 1.2-8.0 |
| Cortisol morning | Low end of range | 2.6 | 01.08.12 |
Summary.
Saliva testing provides direct, practical measurement of the bioactive fraction of multiple hormones, offering insights into real-world hormonal activity that complement information from serum and urine diagnostics. Its non-invasive nature, suitability for at-home collection, and ability to capture dynamic hormonal rhythms have established saliva testing as a versatile and dependable tool for clinicians. From adrenal assessment and HRT monitoring to fertility support and men’s health, salivary diagnostics play a central role in modern endocrine evaluation. Tecan supports laboratories with these applications worldwide with a diverse range of validated saliva immunoassays and automation solutions that enable reliable, efficient salivary hormone testing.
More information.
To explore saliva-based diagnostic solutions and view Tecan’s full portfolio of assays and platforms for hormone analysis, visit:
References
- Mirkin, S. Evidence on the use of progesterone in menopausal hormone therapy. Climacteric, 2018, 21(4), 346-354.
- Carroll JS, Hickey TE, Tarulli GA, Williams M, Tilley WD. Deciphering the divergent roles of progestogens in breast cancer. Nat Rev Cancer. 2017;17(1):54-64.
- Pasqualini JR, Paris J, Sitruk-Ware R, Chetrite G, Botella J. Progestins and breast cancer. J Steroid Biochem Mol Biol. 1998;65(1-6):225-235.
- Kim JJ, Kurita T, Bulun SE. Progesterone action in endometrial cancer, endometriosis, uterine fibroids, and breast cancer. Endocr Rev. 2013;34(1):130-162.
- Sitruk-Ware R, Plu-Bureau G. Progestins and cancer. Endocrinol., 1999, 13(Suppl 4), 3–9.
- Moskowitz, D. A comprehensive review of the safety and efficacy of bioidentical hormones for the management of menopause and related health risks. Med. Rev., 2006, 11(3), 208–223.
- Clarke CL, Sutherland RL. Progestin regulation of cellular proliferation. Rev., 1990, 11(2), 266–301.





